
HonorHealth offers an in-depth look at varicose veins treatment
Sponsored Content | Digital Free Press
Varicose veins, the bulging blood vessels commonly seen in adults over 40, affect an estimated 23% of American adults, according to the American Heart Association.
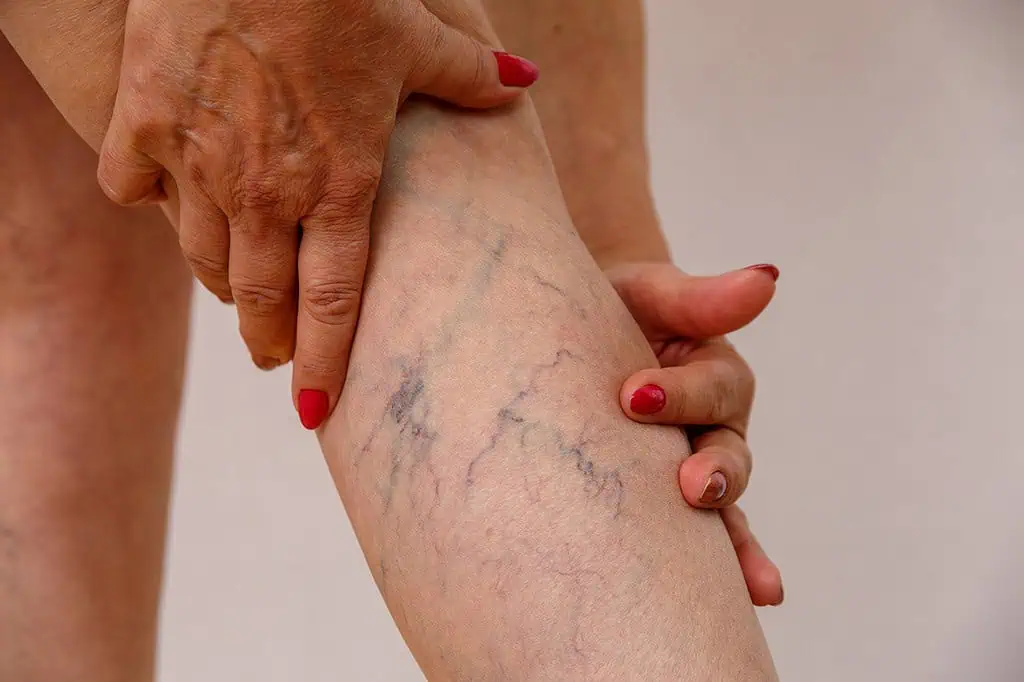
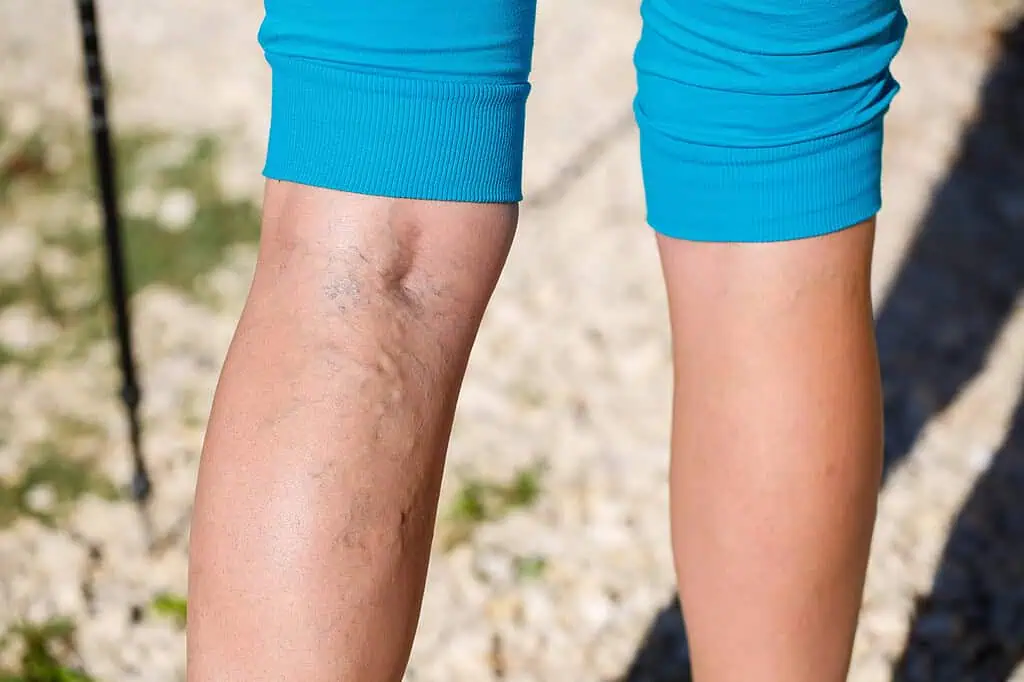
Varicose veins are enlarged, rope-like blood vessels on your thighs, knees and calves that may be purple or red. Spider veins, which are smaller, may also appear due to swollen capillaries.
“Varicose veins tend to occur more often in people who have jobs where they stand for most of the day,” says Alex Westerband, MD, a Scottsdale-based vascular surgeon and independent member of the HonorHealth Medical Staff.
“However, this may be due to stress on veins that are already abnormal. Not everyone who stands all day has varicose veins, but if you were predisposed to getting them, this could be the trigger.”
Dr. Westerband adds that sitting all day can lead to dilation (enlarging of veins) and even blood clots, so he encourages you to get up and move around occasionally, as well as elevating your legs on a stool or cushion when sitting down.
How do varicose veins form?
As you age, tiny valves inside the veins in your legs can begin to wear out or get damaged from either standing too long at a time, too much uninterrupted sitting over the years or other factors.
These damaged valves result in what’s called venous insufficiency – failure of the veins to properly circulate blood. Improper functioning of the valves causes blood to build up inside your veins, leading to vein swelling (what becomes a varicose vein), skin changes and ulcers.

Varicose vein treatment options
“Support hose help keep your veins tucked close to your body and can prevent them from getting progressively dilated over time,” says Dr. Westerband.
“They won’t help with your genetics or hormones, but they will certainly help your symptoms and may reduce the progression of varicosities, swelling and more dilatation of veins.”
Dr. Westerband adds there are minimally invasive procedures to address problem veins if they are painful or causing wounds.
Among the most common procedures is a catheter ablation, which uses radiofrequency or laser energy to heat and close the veins in your legs.
Another option involves the use of a chemical agent to successfully close them.
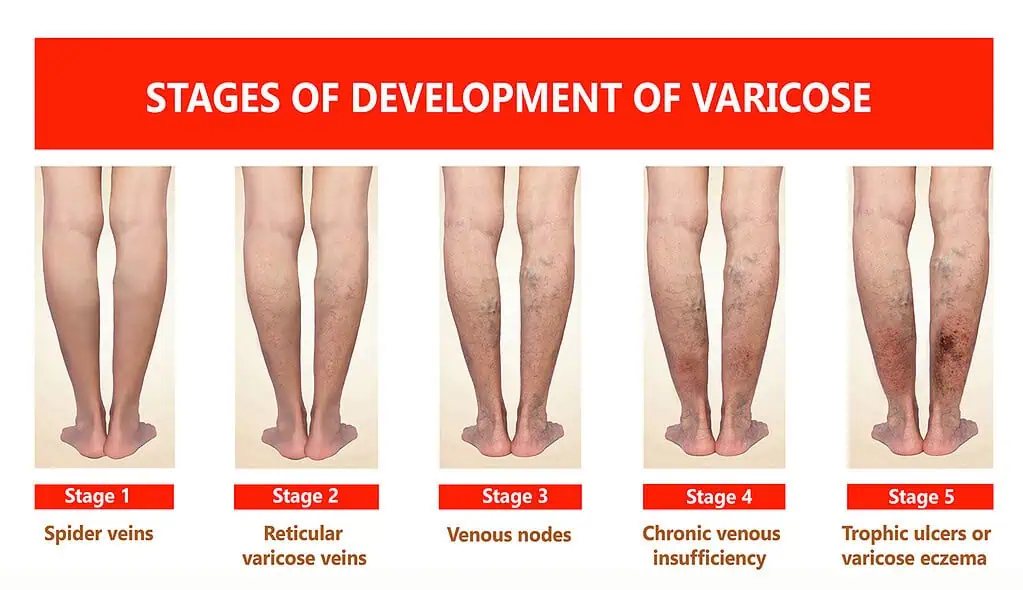
If your legs are swollen, aching, discolored and develop ulcers or wounds, it could be a sign of venous disease. While these may seem cosmetic, sometimes they indicate a more serious underlying vascular condition.
“Our goal is to eliminate abnormal circulation from the bad veins, so they don’t continue to swell or cause skin changes,” Dr. Westerband explains. “Getting you back to feeling your best is our priority.”
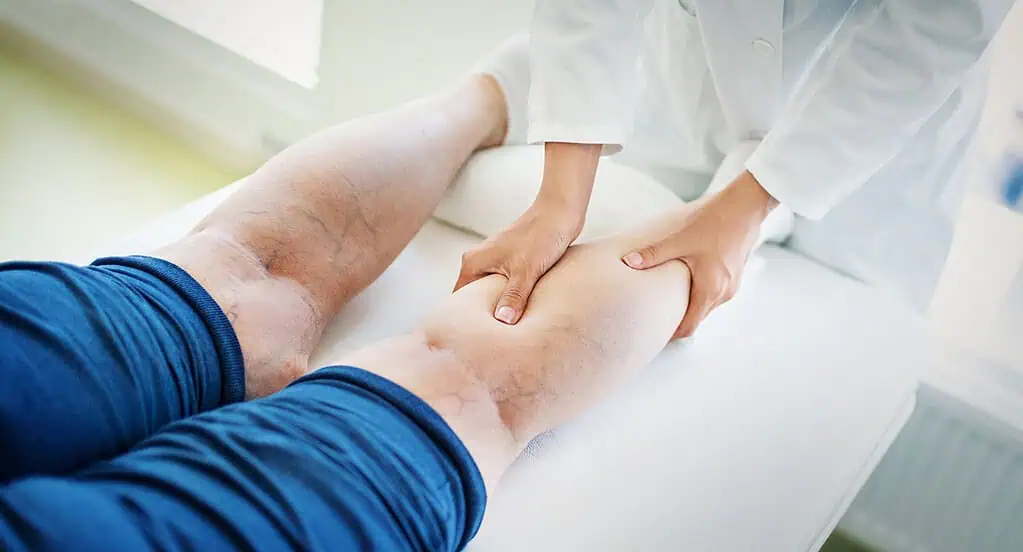
Time to see a vascular specialist
“If your legs hurt when you walk for a brief period of time and the pain ends when you stop or are at rest, this generally points to peripheral arterial disease, or PAD,” says Venkatesh Ramaiah, MD, a vascular surgeon with HonorHealth Heart Care – Vascular and the chief of complex vascular services at HonorHealth Heart Care.
“PAD afflicts almost 20 million people in the U.S. and these symptoms are a sign you should see a vascular specialist to ensure the blood supply to your legs is in the normal range.”
Protecting against and preventing vascular issues
“Good vascular health requires regular checkups with your primary care physician,” advises Hasan Aldailami, MD, a vascular surgeon at HonorHealth.
“They will monitor your blood pressure, cholesterol and lipids (fats, oils and hormones), blood sugar and other important levels in your blood. It’s also essential to follow a healthy, low-fat diet, get modest exercise daily and stop any use of tobacco.”
If you have questions, talk with your doctor or schedule an appointment with an HonorHealth vascular specialist.






